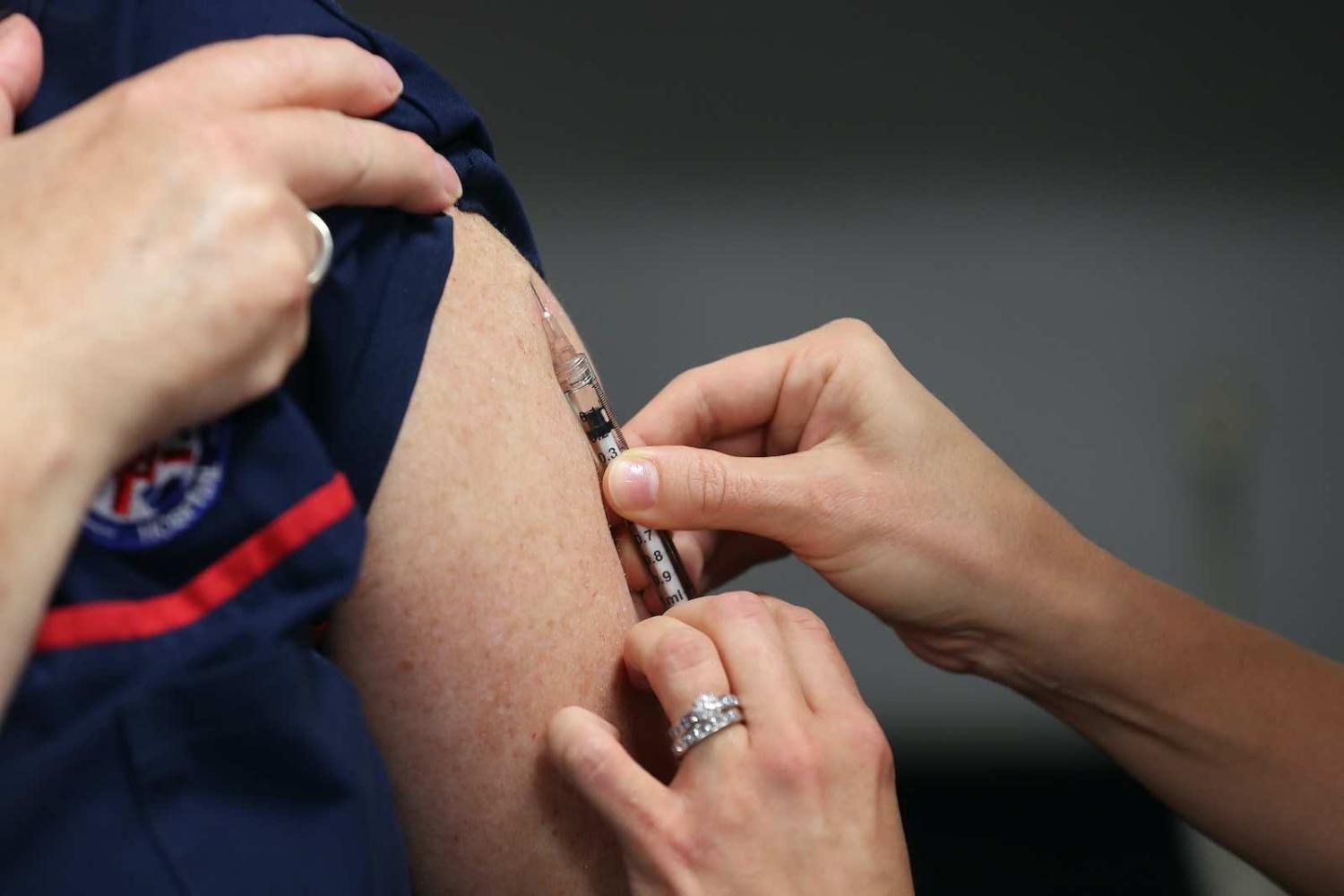
This month, Australia signed a partnership with AstraZeneca, the pharmaceutical company behind the University of Oxford’s proposed Covid-19 vaccine, securing the rights to locally manufacture the vaccine, should it meet safety and efficacy requirements. The Oxford vaccine group has been one of the forerunners in the global race to develop a vaccine against Covid-19, with at least 25 additional vaccine candidates undergoing clinical trials globally, and more than 100 in earlier stages of development.
But as the prospects of a viable vaccine become increasingly within reach, focus is now shifting to what a Covid vaccination strategy should and would look like.
While Australian leaders have set an impressive target of 95% vaccine coverage, limitations in manufacturing and distribution are likely to see a staggered roll-out of any new vaccine. And if so, as we seek to tackle a disease that unashamedly discriminates along lines of socioeconomic class, race and comorbidity, how do we choose who gets vaccinated first?
Three key considerations should guide an effective and equitable vaccine distribution strategy for Australia – and how Australia helps its neighbours.
An imperfect vaccine – letting go of the idea of the silver bullet
Unlike the panacea many are wishing for, any Covid-19 vaccine that reaches the market is likely to be imperfect at best. This requires a paradigm shift in our expectations of a Covid vaccination strategy.
The influenza vaccine is probably the most useful comparison – with effectiveness estimated at between 30–60% (in preventing local doctor or hospital presentations with influenza), and requiring annual vaccination to reflect changes in circulating viral strains, the fluvax is hardly a silver bullet in influenza prevention. Vaccines for coronavirus are likely to face similar limitations in effectiveness and duration of protective effect.
A Covid-19 vaccination strategy will be far from a one-shot wonder and instead will require a long-term commitment to viral suppression.
However, unlike the fluvax, the objective of a Covid-19 vaccination strategy will be to achieve herd immunity, where the proportion of individuals with immunity to the virus is sufficiently high as to halt viral transmission. Estimates to date have indicated that around 2 in 3 people would need to be immune to Covid-19 to achieve herd immunity.
How many people would actually need to receive the vaccine to achieve this level of protective immunity is still unclear, and depends on how effective the vaccine is in generating a protective immune response. Simulations from the US suggest that for a vaccine that is 80% effective, 75% of people would need to be vaccinated. However, a less effective vaccine may need near complete coverage in the community, raising a broader question as to the ethics of mandating vaccination.
Evidence to date also suggests that the immune response to vaccination is likely to wane with time, meaning that regular repeat vaccinations are likely to be necessary. In any sense, a Covid-19 vaccination strategy will be far from a one-shot wonder, and instead will require a long-term commitment to viral suppression.
An unequal virus – who gets the vaccine first?
Viruses may not be able to choose their hosts, but the past six months has unreservedly shown that Covid-19 discriminates. Indeed, data from the US, where the virus has run an aggressive and widely disseminated course, has revealed higher incidence rates of Covid-19 among racial and ethnic minority groups and individuals from lower socioeconomic backgrounds, with concentrated outbreaks occurring in prisons and aged-care facilities.
It is on this backdrop of inequity that focus is now shifting to developing a priority model for distributing a Covid-19 vaccine within Australia. Traditional approaches to planning mass vaccination for pandemics such as influenza have focused on vaccinating those at highest risk of severe infection and mortality (such as those with underlying health conditions) and individuals such as healthcare workers who have high risk of exposure and may serve as vectors for transmission.

Models for a Covid-19 vaccine largely draw from these principles but are undoubtedly shrouded in ethical complexity. Even if a tiered approach for vaccine access is devised, such as to prioritise essential workers or individuals with multiple medical issues, ongoing attention will be necessary to ensure individuals from minority groups are not left behind. This will rely on extensive engagement with community leaders to ensure accessible, culturally appropriate (and correctly translated) information, and will require vaccine distribution to go hand-in-hand with a comprehensive surveillance strategy.
Neighbourly duties – investing in leadership in the Asia-Pacific
Finally, in a time when national introspection has become the norm, Australia has the opportunity to assert itself as a leader and advocate within the Asia-Pacific.
Amid increasing geopolitical uncertainty, Australian leadership in supporting vaccine access and distribution within for Asia-Pacific neighbours is likely to advance broader diplomatic interests, as well as demonstrate a commitment to global health equity.
While Australia has successfully negotiated access to the intellectual property of the Oxford vaccine, a lower “ability-to-pay” and/or lack of manufacturing capacity may preclude similar access for other nations. Australia has indicated a willingness to roll out a working vaccine to Pacific island nations and countries in Southeast Asia. Harnessing this opportunity for collaboration has potential to build stronger Asia-Pacific ties, and at the same time may allow for earlier resumption of travel within the region.
Indeed, as Australia stands on the precipice of the next phase of the Covid challenge, the choices we make in building our vaccine strategy will be best measured by those it leaves behind.